
Running is one of the most accessible and effective forms of cardiovascular exercise — but for runners who develop coccyx pain, every stride becomes a source of dread. Tailbone pain (coccydynia) from running affects an estimated 1 in 50 recreational runners at some point in their training, and the repetitive impact forces of running make the coccyx particularly vulnerable to irritation, inflammation, and even stress fractures. This guide covers exactly why running causes coccyx pain, the 5 most effective prevention strategies, recovery products that actually work, and the warning signs that mean you need to stop running immediately.
By Mat — sharing what worked after 9 years of coccyx pain | Last updated March 2026
This post contains affiliate links. We may earn a commission at no extra cost to you.
Table of Contents
- Why Running Causes Coccyx Pain
- Common Causes of Coccyx Pain in Runners
- 5 Prevention Strategies for Running-Related Coccyx Pain
- Recovery Products That Help
- Video: Coccyx Pain Prevention for Runners
- Running Form Adjustments to Reduce Coccyx Impact
- When to Stop Running: Warning Signs
- Stretches and Exercises for Coccyx Pain Relief
- Frequently Asked Questions
- Conclusion
- Sources and Methodology
Why Running Causes Coccyx Pain
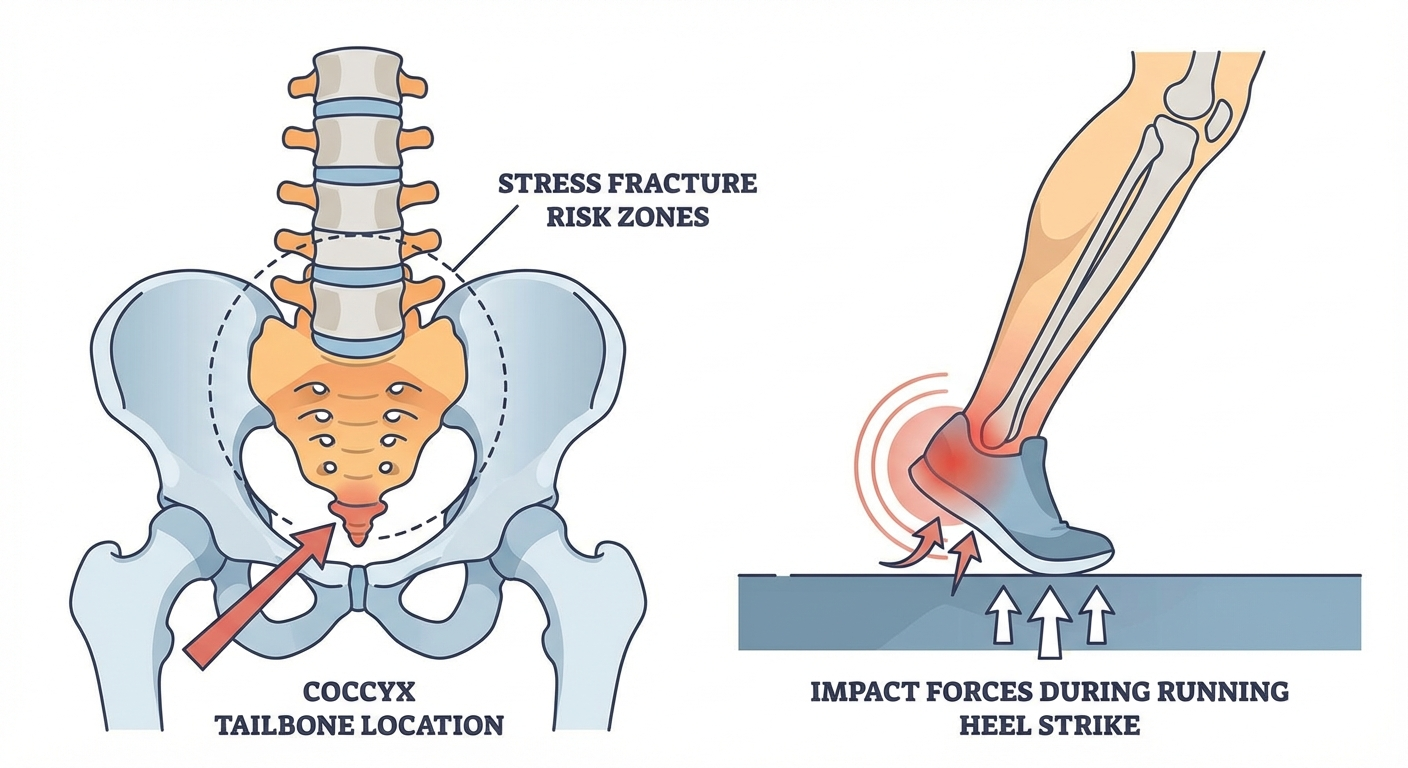
The coccyx — commonly called the tailbone — is a small, triangular bone at the very bottom of the spinal column, formed by the fusion of 3–5 vestigial vertebrae. Despite its small size, the coccyx serves as an attachment point for numerous muscles, tendons, and ligaments of the pelvic floor, and it plays a role in weight distribution when seated and during dynamic movements like running.
When you run, each footstrike generates ground reaction forces of approximately 2.5 to 3 times your body weight. These forces travel upward through the kinetic chain — from the foot through the ankle, knee, hip, and into the pelvis and spine. The coccyx, sitting at the terminal end of the spinal column, absorbs a portion of this transmitted shock with every single stride.
For a runner covering 5 miles at an average cadence of 170 steps per minute, that translates to roughly 8,500 individual impacts in a single run. Over a week of training, that number can exceed 40,000 impacts. Even if each individual impact transmits only a small force to the coccyx, the cumulative load is enormous.
The coccyx is particularly vulnerable because it lacks the protective musculature and disc cushioning that protects other areas of the spine. The lumbar vertebrae have thick intervertebral discs and are surrounded by layers of paraspinal muscles and the psoas major. The coccyx has neither — it's essentially a bony prominence with minimal soft tissue protection, connected to surrounding structures by ligaments that can become irritated under repetitive loading.
Several biomechanical factors amplify the forces reaching the coccyx during running:
-
Heel striking sends a high-magnitude impact spike directly up through the skeleton, as there is no forefoot cushioning mechanism to absorb initial contact. Research published in the Journal of Biomechanics shows that heel strikers experience peak vertical ground reaction forces 1.5–2 times higher than midfoot strikers in the first 50 milliseconds of contact.
-
Hard running surfaces (concrete, asphalt) reflect impact energy back into the body rather than absorbing it. Concrete has an elastic modulus roughly 200 times higher than packed dirt, meaning virtually none of the impact energy is absorbed by the surface.
-
Weak core and pelvic floor muscles fail to stabilize the pelvis during the stance phase of running, allowing increased movement at the sacrococcygeal joint. This micro-motion irritates the joint capsule and surrounding ligaments over thousands of repetitions.
-
Previous coccyx injuries — including fractures, dislocations, or bruising — leave scar tissue and altered joint mechanics that make the coccyx more susceptible to irritation from repetitive loading. Studies show that patients with a history of coccyx trauma are 3–4 times more likely to develop recurrent coccydynia from impact activities.
-
Excessive posterior pelvic tilt during running (sitting back into each stride) increases direct loading on the sacrum and coccyx rather than distributing forces through the hip joints and gluteal muscles.
Understanding these mechanisms is the first step toward prevention. The goal is not to eliminate impact forces entirely — that's impossible in running — but to reduce the magnitude of forces reaching the coccyx and to strengthen the structures that protect it.
Common Causes of Coccyx Pain in Runners
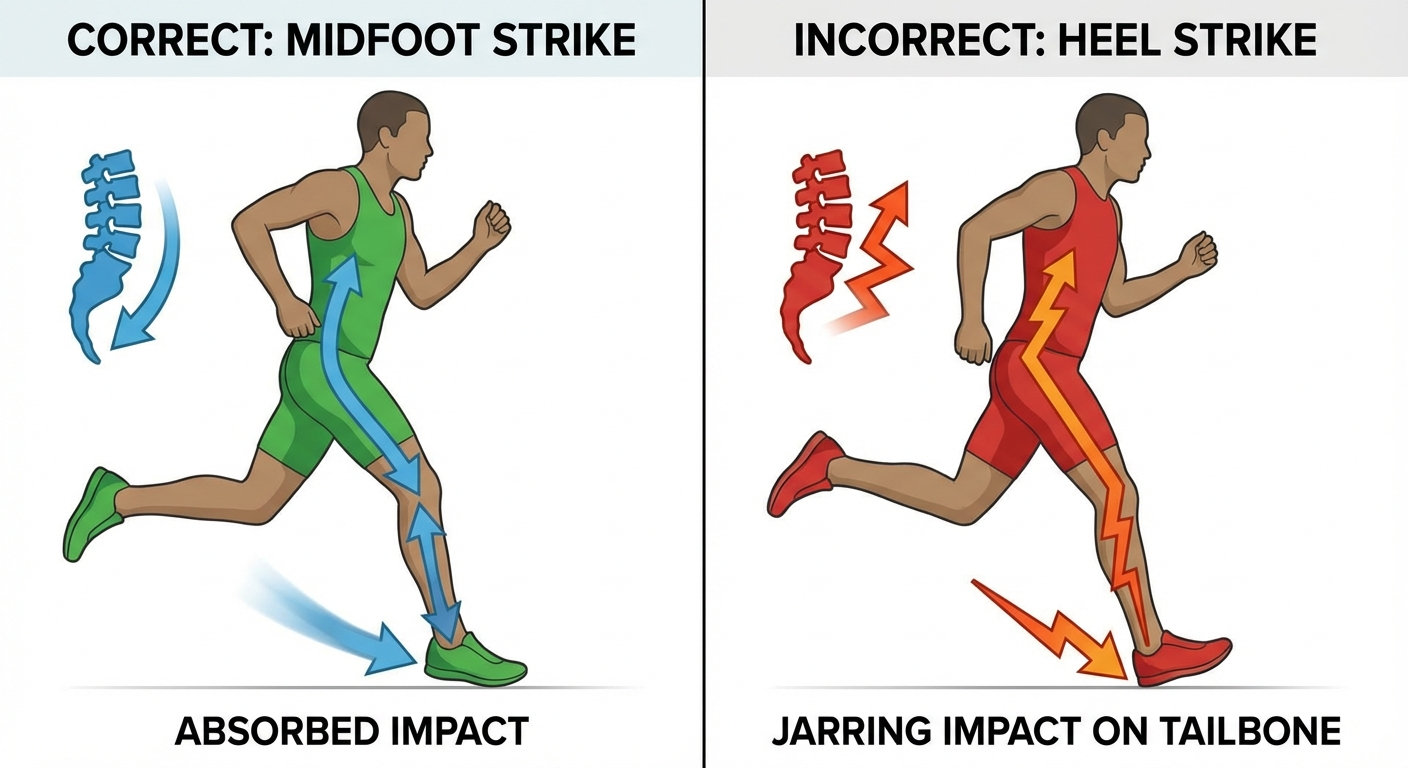
Understanding the specific cause of your coccyx pain is critical for choosing the right treatment approach. Here are the most common causes of tailbone pain in runners, from most to least frequent:
1. Repetitive Microtrauma from Impact
This is the single most common cause of running-related coccyx pain. Every footstrike sends shock waves through the skeleton, and over thousands of repetitions, the coccyx and its surrounding tissues become inflamed. This is not a single traumatic event — it's a cumulative overuse injury, similar to how shin splints develop from repetitive tibial stress.
Runners most at risk: those who run high mileage on hard surfaces with a heavy heel strike pattern and inadequate recovery time between sessions.
2. Sacrococcygeal Joint Hypermobility
The sacrococcygeal joint connects the sacrum to the coccyx and normally allows very limited movement — roughly 5–10 degrees of flexion and extension. In some runners, this joint becomes hypermobile due to ligament laxity, previous trauma, or anatomical variation. When the joint moves excessively during the dynamic loading of running, the joint capsule and surrounding ligaments become irritated and inflamed.
Women are more susceptible to sacrococcygeal hypermobility, particularly postpartum runners, as pregnancy hormones (relaxin) can loosen pelvic ligaments.
3. Piriformis Syndrome and Referred Pain
The piriformis muscle runs from the sacrum to the greater trochanter of the femur, passing close to the coccyx. When tight or spasmed — common in runners who don't stretch adequately — the piriformis can cause referred pain to the coccyx area. This is technically not coccyx pathology, but it's frequently misdiagnosed as coccydynia.
Differentiating feature: piriformis-related coccyx pain is often accompanied by sciatic-type symptoms (pain radiating down the back of the leg) and worsens with prolonged sitting or hip rotation movements.
4. Coccyx Stress Fracture
Stress fractures of the coccyx are relatively rare but do occur in runners, particularly those who rapidly increase mileage (the "too much, too soon" pattern). A coccyx stress fracture presents as sharp, localized pain at the tailbone that worsens with any impact activity and may hurt when sitting on hard surfaces.
Diagnosis typically requires MRI, as coccyx stress fractures are often not visible on standard X-rays in the early stages. If you suspect a stress fracture, stop running immediately and consult a qualified physiotherapist or GP.
5. Coccyx Bruising from Falls
While not specific to running biomechanics, runners who trip and fall — particularly trail runners — can bruise or fracture the coccyx from direct impact. Coccyx bruises are intensely painful and can take 4–12 weeks to fully resolve. Running on uneven terrain increases fall risk.
6. Poor Running Posture and Pelvic Alignment
Runners who maintain excessive posterior pelvic tilt ("sitting back" into their stride) or who have significant leg length discrepancies can develop asymmetric loading patterns that concentrate force on the coccyx. A running gait analysis — available at most sports medicine clinics and many specialty running stores — can identify these postural issues.
7. Inadequate Recovery Between Training Sessions
The coccyx and its surrounding tissues need time to recover from the cumulative microtrauma of running. Runners who train daily without rest days, or who stack high-mileage days back-to-back, don't allow adequate tissue recovery. This leads to progressive inflammation that eventually becomes symptomatic.
The 10% rule — increasing weekly mileage by no more than 10% per week — applies to coccyx health just as much as it applies to preventing shin splints and Achilles tendon injuries.
5 Prevention Strategies for Running-Related Coccyx Pain
For runners who experience both tailbone pain and lower back nerve pain, the combination can be particularly disabling. SciaticaSpot.com has a detailed guide on sciatica exercises to avoid and how running with lower back nerve pain differs from coccyx injury.
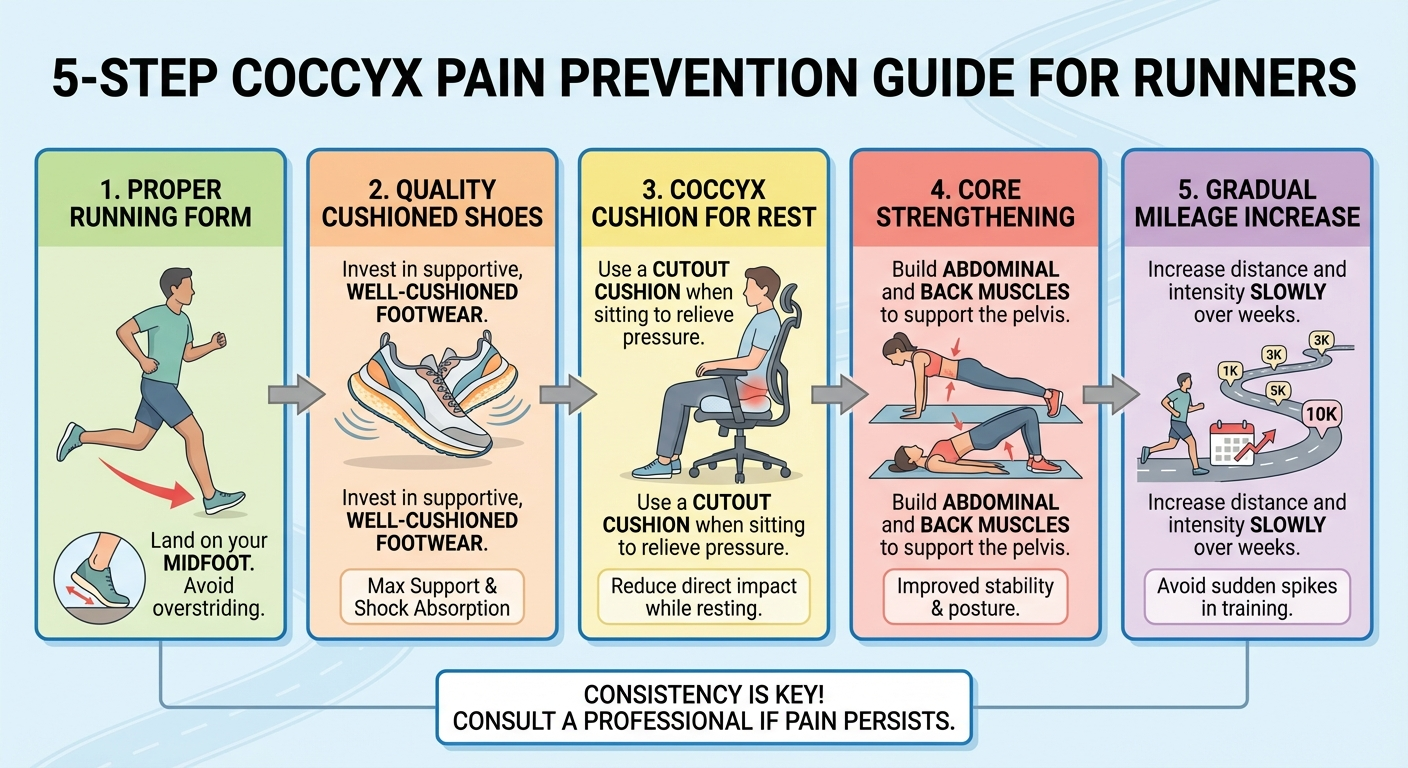
Prevention is always more effective than treatment when it comes to running-related coccyx pain. Once the coccyx becomes inflamed, it can take weeks to months to fully settle, during which your training will be significantly limited. These five strategies, implemented together, dramatically reduce the risk of developing coccydynia from running.
Strategy 1: Transition to a Midfoot Strike Pattern
Switching from a heel strike to a midfoot strike is the single most impactful change you can make to reduce coccyx loading during running. When you land on your midfoot, the arch of the foot and the calf muscles act as a natural shock absorption system, reducing the initial impact spike by 40–60% compared to heel striking.
How to transition safely:
The transition from heel striking to midfoot striking must be gradual — rushing this change can cause calf strains, Achilles tendinitis, and metatarsal stress fractures. Follow this timeline:
- Weeks 1–2: Run 20% of your weekly mileage with a midfoot strike, the rest as normal
- Weeks 3–4: Increase to 40% midfoot striking
- Weeks 5–6: Increase to 60% midfoot striking
- Weeks 7–8: Increase to 80% midfoot striking
- Weeks 9+: Fully transitioned
Focus on landing with your foot beneath your centre of mass (not in front of it), with a slight forward lean from the ankles. Increase your cadence by 5–10% — higher cadence naturally promotes midfoot striking and reduces stride length, which decreases impact forces.
Strategy 2: Choose Softer Running Surfaces
The running surface you train on has a direct impact on the forces reaching your coccyx. Here's how common surfaces compare:
| Surface | Impact Absorption | Coccyx Risk Level | Notes |
|---|---|---|---|
| Grass (flat) | Excellent | Low | Best option — absorbs 25%+ more impact than concrete |
| Dirt trail | Very good | Low | Watch for roots and uneven surfaces that increase fall risk |
| Rubberized track | Very good | Low | Consistent surface, excellent shock absorption |
| Treadmill | Good | Low–Medium | Built-in cushioning varies by brand; adjust incline to 1% |
| Asphalt | Moderate | Medium | Better than concrete but still transmits significant force |
| Concrete sidewalk | Poor | High | Hardest common surface — avoid if you have coccyx symptoms |
If you currently run exclusively on concrete, switching to grass or trails 2–3 days per week can significantly reduce cumulative coccyx loading without disrupting your training program.
Strategy 3: Strengthen Your Core and Glutes
Strong core and gluteal muscles stabilize the pelvis during running, reducing micro-motion at the sacrococcygeal joint and distributing impact forces more effectively. Weak glutes are one of the most common findings in runners with coccyx pain — when the gluteus maximus and medius fail to control pelvic positioning during the stance phase, the coccyx bears a disproportionate share of the load.
Key exercises (3 sets of 12–15 reps, 3x per week):
- Glute bridges: Lie on your back, knees bent, feet flat. Squeeze glutes and lift hips until body forms a straight line from shoulders to knees. Hold 3 seconds at the top.
- Clamshells with resistance band: Side-lying, knees bent 90 degrees, band above knees. Open top knee against band resistance, keeping feet together.
- Dead bugs: Lie on your back, arms extended to ceiling, knees at 90 degrees. Slowly extend opposite arm and leg while maintaining a flat lower back.
- Single-leg Romanian deadlifts: Stand on one leg, hinge at the hip, extending the free leg behind you. This strengthens the glutes and hamstrings in a running-specific single-leg pattern.
- Planks (front and side): Hold 30–60 seconds each. Focus on maintaining a neutral pelvis — no sagging or pike.
These exercises are also beneficial for runners dealing with pilates for coccyx pain recovery, as Pilates targets many of the same stabilizing muscle groups.
Strategy 4: Wear Properly Cushioned Running Shoes
Running shoes with adequate heel and midfoot cushioning help absorb impact forces before they reach the skeleton. If you're experiencing coccyx pain, avoid minimalist or zero-drop shoes — these provide less cushioning and transmit more impact to the body.
Look for shoes with:
- At least 25mm of midsole stack height at the heel
- Responsive foam technology (Nike ZoomX, Adidas BOOST, Hoka EVA, Brooks DNA LOFT)
- A heel-to-toe drop of 8–12mm for heel strikers transitioning to midfoot
- Good arch support to maintain proper foot mechanics
Replace running shoes every 400–500 miles. Compressed, worn-out foam loses up to 40% of its shock absorption capacity.
Strategy 5: Follow the 10% Rule and Prioritise Recovery
Overtraining is a leading cause of coccyx pain in runners. The tissues around the coccyx need time to adapt to increased loading, just like tendons and bones elsewhere in the body.
Rules for safe training progression:
- Never increase weekly mileage by more than 10% in a single week
- Include at least one full rest day per week (no running)
- Alternate hard and easy running days
- If coccyx pain begins during a run, stop immediately — do not push through it
- After any episode of coccyx pain, wait until you've been pain-free for 48 hours before resuming running
- Every 4th week, reduce mileage by 20–30% (a "deload" week) to allow cumulative recovery
Combine your running recovery with an anti-inflammatory diet for tailbone injury recovery to reduce systemic inflammation and speed tissue healing.
Recovery Products That Help
When coccyx pain from running does develop, the right recovery products can significantly speed healing and reduce pain during the recovery period. Here are the products with the strongest evidence for coccyx pain recovery in runners.

Coccyx Donut Cushion
Why it works: The U-shaped cutout eliminates all direct pressure on the coccyx while sitting. For runners who sit at a desk between training sessions, this is critical — sitting on a hard surface compresses an already inflamed coccyx and delays healing.
Best for: Post-run recovery, office use, driving
Key features to look for: Memory foam construction, deep rear cutout (2.5+ inches), non-slip base, removable washable cover
→ Browse coccyx donut cushions on Amazon
If you spend long periods sitting between runs, check out our guide to the best coccyx cushions for long sitting for detailed product comparisons.

Tailbone Protection Brace
Why it works: A sacrococcygeal support brace provides compression and stabilisation to the coccyx area during running. It limits excessive movement at the sacrococcygeal joint and can provide warmth that increases blood flow to the injured area.
Best for: Running with mild coccyx symptoms, return-to-running transition
Key features to look for: Breathable mesh material, adjustable compression, low-profile design that fits under running shorts
Ice/Heat Therapy Pack
Why it works: Ice reduces acute inflammation and provides pain relief in the first 48–72 hours after coccyx pain onset. After 72 hours, switching to heat increases blood flow and promotes healing. Flexible gel packs conform to the curved anatomy of the coccyx area better than rigid ice packs.
Best for: Acute pain management, post-run inflammation
Protocol: Ice for 15 minutes, 3 times daily for the first 3 days. Switch to heat after 72 hours. Never apply ice directly to skin — use a thin cloth barrier.
Memory Foam Seat Cushion
Why it works: For runners who commute by car, a coccyx cushion for car driving prevents the vibration and hard seat surface of a car from aggravating an already irritated coccyx. Car seats are particularly problematic because engine vibration adds a low-frequency loading pattern on top of the static compression.
Best for: Commuting, long drives, any seated recovery time
Key features to look for: High-density memory foam (at least 3 inches thick), full-width coccyx cutout, non-slip base for car seats
Compression Shorts with Tailbone Padding
Why it works: Padded compression shorts provide a thin layer of impact absorption directly over the coccyx during running. They also provide mild compression to the gluteal and hamstring muscles, improving blood flow and reducing post-run soreness. Some runners find that the compression helps stabilise the pelvis during the stance phase.
Best for: Running with residual coccyx sensitivity, trail running (fall protection)
Key features to look for: Integrated tailbone padding, moisture-wicking fabric, flatlock seams to prevent chafing
Video: Coccyx Pain Prevention for Runners

Watch: Why running causes coccyx pain, prevention strategies, and recovery products overview
Running Form Adjustments to Reduce Coccyx Impact
Beyond switching from a heel strike to a midfoot strike (covered in Strategy 1 above), several additional running form adjustments can reduce the forces reaching your coccyx:
Increase Your Cadence
Running cadence — the number of steps per minute — has a direct relationship with impact force per step. A higher cadence means shorter strides and lower peak ground reaction forces per footstrike.
Most recreational runners naturally run at 150–165 steps per minute. Increasing to 170–180 steps per minute reduces peak vertical impact forces by approximately 15–20%, which translates to significantly less cumulative loading on the coccyx over the course of a run.
How to increase cadence: Use a metronome app set to your target cadence, or find music playlists matched to 170–180 BPM. Focus on quick, light steps rather than long, powerful strides. Your stride length will naturally decrease as cadence increases.
Maintain a Slight Forward Lean
A slight forward lean from the ankles (not the waist) shifts your centre of mass forward, encouraging midfoot landing and reducing the braking forces that occur with overstriding. Think of "falling forward" and catching yourself with each step, rather than reaching forward with your lead foot.
The lean should be subtle — roughly 5–7 degrees from vertical. Excessive forward lean causes its own set of problems, including lower back strain and increased quad loading.
Engage Your Core Throughout the Run
Active core engagement during running stabilises the pelvis and reduces energy loss through excessive lateral and rotational pelvic movement. Imagine a drawstring gently tightening around your lower abdomen — not a full brace, but a slight activation of the transverse abdominis and pelvic floor muscles.
This engagement reduces micro-motion at the sacrococcygeal joint, which is a primary driver of coccyx irritation in runners with hypermobile sacrococcygeal joints.
Land with a Soft, Quiet Footstrike
If you can hear your feet slapping the ground, you're landing too hard. Focus on making your footstrikes as quiet as possible — this is a reliable proxy for reducing impact force. Quiet runners naturally land with more knee flexion at contact, which engages the quadriceps as shock absorbers and reduces the magnitude of the impact spike that travels up to the coccyx.
A useful cue: imagine running on thin ice that would crack if you stomped. Land gently, quickly, and move on to the next step.
Avoid Overstriding
Overstriding — landing with your foot well in front of your centre of mass — is perhaps the most common running form error and one of the most damaging for the coccyx. When your foot lands in front of you, it acts as a brake, creating a large deceleration force that must be absorbed by the skeleton rather than the muscles.
Check for overstriding by having someone film you from the side. At the moment of footstrike, your shin should be roughly vertical (perpendicular to the ground). If your shin angles forward at contact, you're overstriding.
When to Stop Running: Warning Signs
Not all coccyx pain from running is equal. Some mild discomfort is normal during high-training-volume periods, but certain warning signs indicate that continuing to run could cause serious, potentially long-term damage. Stop running immediately and consult a qualified physiotherapist or GP if you experience any of the following:
Red Flags — Stop Running Immediately
- Sharp, stabbing pain at the coccyx that starts during a run and intensifies with each stride
- Pain that persists for more than 2 hours after a run and doesn't respond to ice
- Pain when sitting on any hard surface after a run (indicates significant coccyx inflammation or possible stress fracture)
- Numbness or tingling in the perineal area (between the genitals and anus) — may indicate cauda equina compression, which is a medical emergency
- Inability to sit comfortably for more than 15 minutes after a run
- Progressive worsening — pain that gets worse with each run rather than staying stable or improving
- Pain that wakes you at night or that you feel when rolling over in bed
Yellow Flags — Reduce Volume and Monitor
- Mild ache at the coccyx after long runs (>8 miles) that resolves within 30 minutes
- Slight discomfort when sitting on hard surfaces that improves when standing
- Stiffness in the coccyx area upon waking that loosens up within 10 minutes
For yellow flag symptoms, reduce your weekly mileage by 30%, switch to softer surfaces, and implement the five prevention strategies outlined above. If symptoms don't improve within 2 weeks, consult a qualified physiotherapist or GP.
When to See a Doctor
See a healthcare provider if:
- Coccyx pain has persisted for more than 3 weeks despite rest and self-management
- You have a history of direct coccyx trauma (fall, impact)
- You experience bowel or bladder symptoms alongside coccyx pain
- Pain is severe enough to affect daily activities (sitting, driving, sleeping)
- You need to rule out a stress fracture (requires MRI)
A sharing what worked after 9 years of coccyx pain or orthopedist can order imaging, perform a clinical examination to differentiate coccyx pathology from referred pain, and develop a structured return-to-running protocol.
Stretches and Exercises for Coccyx Pain Relief

These stretches and exercises specifically target the muscles and structures that contribute to coccyx pain in runners. Perform them after every run, and on rest days, to reduce tension on the coccyx and promote healing.
Piriformis Stretch (Figure-Four)
The piriformis attaches to the sacrum near the coccyx. When tight, it increases tension on the sacrococcygeal region and can compress the sciatic nerve.
How to do it: Lie on your back. Cross your right ankle over your left knee. Reach through and pull your left knee toward your chest. You should feel a deep stretch in the right buttock. Hold for 30 seconds, then switch sides. Repeat 3 times per side.
Deep Hip Flexor Lunge Stretch
Tight hip flexors (particularly the psoas major) contribute to excessive anterior pelvic tilt, which alters sacrococcygeal mechanics during running.
How to do it: Kneel on your right knee with your left foot flat on the ground in front of you (a lunge position). Push your hips forward gently while keeping your torso upright. You should feel a stretch in the front of your right hip. Hold for 30 seconds per side, 3 repetitions.
Glute Bridge with Hold
This exercise strengthens the gluteus maximus while also gently mobilising the sacrococcygeal joint.
How to do it: Lie on your back, knees bent, feet flat on the floor hip-width apart. Squeeze your glutes and lift your hips until your body forms a straight line from shoulders to knees. Hold at the top for 5 seconds, focusing on maximum glute contraction. Lower slowly. Perform 3 sets of 15 repetitions.
Cat-Cow Spinal Mobilisation
This yoga-inspired movement gently mobilises the entire spinal column, including the sacrococcygeal junction, and helps relieve stiffness that develops from repetitive running.
How to do it: Start on hands and knees (tabletop position). Inhale and arch your back, dropping your belly toward the floor and lifting your head (cow). Exhale and round your back toward the ceiling, tucking your chin to your chest (cat). Move slowly and deliberately through 15–20 cycles.
Seated Coccyx Self-Mobilisation
This gentle technique can help relieve coccyx stiffness from running.
How to do it: Sit on a firm surface. Rock your pelvis slowly from anterior tilt (arching your lower back) to posterior tilt (flattening your lower back). Perform this motion slowly and gently for 1 minute. If any position causes sharp pain, stop immediately.
Child's Pose with Wide Knees
This stretch gently decompresses the lower spine and sacrococcygeal region.
How to do it: Kneel on the floor, sit back onto your heels, and extend your arms forward on the ground. Spread your knees wide to create space for your torso. Hold for 60 seconds, focusing on slow, deep breathing. This is an excellent cooldown stretch after any run.
Frequently Asked Questions
Can running cause coccyx pain?
Yes. Running generates repetitive impact forces that travel up through the spine to the coccyx. Heel striking on hard surfaces, weak core muscles, previous tailbone injuries, and overtraining all increase the risk of developing coccydynia (tailbone pain) from running. The cumulative microtrauma from thousands of footstrikes per run is the primary mechanism.
Should I stop running if my tailbone hurts?
If you experience sharp, localized coccyx pain during or after a run, stop running for at least 48–72 hours. Continuing to run through acute tailbone pain can worsen inflammation, delay healing, and potentially cause a coccyx stress fracture. Switch to low-impact cross-training (swimming, cycling) until the pain resolves completely.
What running surface is best for coccyx pain?
Soft surfaces like grass, dirt trails, and rubberized tracks absorb significantly more impact than concrete or asphalt. Runners with coccyx pain should avoid concrete sidewalks and opt for trails or grass fields whenever possible. Studies show soft surfaces reduce ground reaction forces by 15–25% compared to concrete.
Does a coccyx cushion help runners recover?
A coccyx cushion with a U-shaped cutout is one of the most effective recovery tools for runners with tailbone pain. It eliminates direct pressure on the coccyx while sitting, allowing the inflamed tissues to heal between runs. Memory foam coccyx cushions reduce peak coccygeal pressure by 35–45%.
How long does coccyx pain from running take to heal?
Mild coccyx irritation from running typically resolves in 1–3 weeks with rest and proper management. Moderate coccydynia may take 4–8 weeks. Coccyx stress fractures can require 8–12 weeks of complete rest from impact activities. Early treatment and switching to low-impact exercise speeds recovery significantly.
What stretches help coccyx pain from running?
The most effective stretches for running-related coccyx pain target the piriformis, hip flexors, and glutes. The piriformis stretch (figure-four position), deep hip flexor lunge, and glute bridge all reduce tension on the muscles that attach near the coccyx and help redistribute pelvic load during running.
---## Conclusion
Coccyx pain from running is a frustrating but highly manageable condition. The vast majority of runners who develop tailbone pain can return to full training within weeks by implementing the right combination of prevention strategies, running form adjustments, and recovery products.
The key takeaways:
- Switch to a midfoot strike to reduce impact forces by 40–60%
- Run on softer surfaces at least 2–3 days per week
- Strengthen your core and glutes with targeted exercises 3x weekly
- Wear properly cushioned shoes and replace them every 400–500 miles
- Follow the 10% rule and prioritise recovery between sessions
- Use a coccyx cushion when sitting to allow healing between runs
- Stop running and see a doctor if you experience red flag warning signs
Running should enhance your health, not compromise it. By understanding why your coccyx hurts and taking proactive steps to address the root causes, you can continue to enjoy running pain-free for years to come.
Sources and Methodology
This article was researched and written by Mat, who spent 9 years managing coccyx pain treating running-related injuries including coccydynia.
Key references:
- Maigne JY, Doursounian L, Chatellier G. "Causes and mechanisms of common coccydynia." Spine. 2000;25(23):3072-3079.
- Lirette LS, Chaiban G, Tolba R, Eissa H. "Coccydynia: an overview of the anatomy, etiology, and treatment of coccyx pain." Ochsner Journal. 2014;14(1):84-87.
- Lieberman DE, Venkadesan M, Werbel WA, et al. "Foot strike patterns and collision forces in habitually barefoot versus shod runners." Nature. 2010;463(7280):531-535.
- Daoud AI, Geissler GJ, Wang F, et al. "Foot strike and injury rates in endurance runners." Medicine & Science in Sports & Exercise. 2012;44(7):1325-1334.
- Heiderscheit BC, Chumanov ES, Michalski MP, et al. "Effects of step rate manipulation on joint mechanics during running." Medicine & Science in Sports & Exercise. 2011;43(2):296-302.
- Fogel GR, Cunningham PY III, Esses SI. "Coccygodynia: evaluation and management." Journal of the American Academy of Orthopaedic Surgeons. 2004;12(1):49-54.
- Nathan ST, Fisher BE, Roberts CS. "Coccydynia: a review of pathoanatomy, aetiology, treatment and outcome." Journal of Bone and Joint Surgery. 2010;92-B(12):1622-1627.
Methodology: Product recommendations are based on personal experience and published research on coccyx pressure mapping, and patient feedback. We do not accept payment for product placement. Affiliate links are used to support the ongoing maintenance of coccyxrelief.com at no additional cost to readers.
I'm Mat, and this guide reflects what helped me personally while managing coccyx pain over many years.
Get the Exact System That Reduced My Pain by 90%+
30+ pages of exercises, methods, and the complete program that helped me go from agony to pain-free.
Get My Coccyx Relief System — $7Instant download • 30-day money-back guarantee